Category: Protection & Common STD’s
February 24th, 2017 by admin
What are sexually transmitted diseases?
The names “sexually transmitted disease” or “sexually transmitted infection” may be a lot more straightforward than the old term “venereal disease,” but they still bear some explanation. A sexually transmitted disease (STD) is any disease passed from person to person by sexual contact. Sexual contact includes all forms of penetrating intercourse, oral sex and a wide range of activities that might be described as sex play or foreplay. Some STDs can be passed through mere skin-to-skin contact; others require contact with infected body fluids such as blood, semen, saliva or vaginal secretions. A number of STDs can also be passed from mother to child during pregnancy or at birth. There are more than two dozen different STDs , which can be caused by very different microbes. Many–chlamydia and gonorrhea, to name two of the most common–are caused by bacteria. Some, such as herpes and HIV/AIDS, are caused by viruses. Still others are caused by parasites and other microorganisms.
Once and for all, is it true that some STDs actually can be spread through contact with things such as toilet seats and hot tubs?
It’s highly unlikely that any STD would be spread by way of an inanimate object or surface such as a tanning bed or a toilet seat. The obvious exceptions are objects used in penetrative sex (sex toys such as dildos) and needles used for injecting drugs. Towels or other household objects also may be involved in the spread of some infections, particularly parasites such as lice.
Many of the bacteria and viruses responsible for STDs don’t survive long outside the body. In addition, some of them require friction in order to gain entry into the skin or mucous membranes of a new host. (Mucous membranes are the soft, moist tissue of areas such as the inside of the mouth or vagina.) Lastly, with reference to toilet seats, you have to remember that the thick skin of the buttocks and thighs is not especially susceptible to infection.
Hot tubs, too, have sometimes been rumored to be a source of STDs. But the chlorine and mineral salts used in these tubs are generally deadly to STD microbes. As an editorial in the Journal of the American Medical Association once put it, the question of whether you can get an STD from a hot tub depends entirely on what you’re doing in the tub.
Who is at risk of getting an STD?
Anyone. The risk of acquiring an STD has to do with what you do, not who you are. Lots of people have the idea that STDs are unusual diseases that affect only a small segment of the population. On the contrary, STDs are among the most widespread kinds of infectious disease, being outranked only by ubiquitous illnesses such as the common cold. According to a recent report by the Kaiser Family Foundation, there are an estimated 15 million new sexually transmitted infections every year in the United States. Taking the U.S. population as a whole, the odds that a person will contract an STD over the course of a lifetime are one in four. One reason for these high rates is that human beings give STDs lots of opportunities to spread. Consider this: Worldwide, according to the World Health Organization, intercourse takes place 42 billion times per year. That works out to 1300 ejaculations per second.
How would I know if I had an STD?
Identifying STDs is not always easy. Given that there are two dozen STDs, it’s impossible to include every symptom in a short list, but here are some of the most common ones:
- – Sores, blisters, bumps or rashes on or near the genitals
- – Painful urination, or an unusual discharge with the urine
- – Abnormal vaginal discharge or strong odor
- – Bleeding between menstrual periods
- – Pain in the lower abdomen or swollen lymph nodes in the groin
One of the big problems in controlling the spread of STDs, however, is that in lots of people these diseases do not cause symptoms. (Medical texts often use the term “asymptomatic.”) In addition, several STDs cause symptoms that are quite subtle and hard to recognize. In many cases, then, the only way to identify an STD is with a diagnostic test.
Do STDs pose any long-term health risks?
Sometimes. While some sexually transmitted infections may resolve quickly without complications, others play a role in problems such as the development of cervical cancer, liver disease and reproductive tract disorders that can impair a person’s ability to have children. Among the most serious consequences of STDs is the risk they pose to infants who are exposed in the womb or at birth. Many of these children may suffer serious mental retardation or life-threatening illness. Lastly, of course, the most lethal STD is HIV/AIDS, which is still incurable.
What are the most common STDs?
When surveyed, most Americans name HIV/AIDS along with gonorrhea as the most common STDs, but actually these conditions are not the most widespread. The sexually transmitted diseases with the largest number of new cases per year are HPV and trichomoniasis, both of which are estimated to afflict 5 million persons per year. Because both of these infections can be cured, however, a large proportion of those infected in a given year will be clear of infection by the next year.
By contrast, some of the viral infections, such as herpes and human papillomavirus (HPV), are not curable. They persist for the life of the person infected, so the total number of infected persons (prevalence) grows each year. The current prevalence for both herpes and HPV is estimated in the tens of millions in the United States.
Posted in Protection & Common STD’s
February 9th, 2017 by admin
I’ve heard of chlamydia but don’t know anything about it. What is it?
 Chlamydia is a unique type of bacterium that attaches itself to healthy cells and draws on these cells for the elements necessary to grow and invade other cells. It does not belong to the group of bacteria that are normally found in the genital tract but is transmitted sexually through contact with secretions such as semen and vaginal fluids.
Chlamydia is a unique type of bacterium that attaches itself to healthy cells and draws on these cells for the elements necessary to grow and invade other cells. It does not belong to the group of bacteria that are normally found in the genital tract but is transmitted sexually through contact with secretions such as semen and vaginal fluids.
Chlamydia is found in 3 to 20% of men and women, depending on the population sampled. In up to 85% of women and 40% of men, chlamydial infection causes no symptoms. However, even when asymptomatic, chlamydia can result in serious long-term problems, principally damage to the female reproductive organs.
What kind of reproductive damage are we talking about?
Chlamydia is mainly implicated in damage to the fallopian tubes. This, in turn, can lead to infertility (defined as the inability to conceive after 12 months of trying). And because chlamydia is so common–with an estimated 4 milllion new cases each year–it’s considered one of the leading preventable causes of infertility.
Chlamydia also has been implicated in ectopic pregnancy–a pregnancy in which the fetus implants outside the uterus, usually in the fallopian tube. This is a potentially deadly medical condition that requires emergency care; it’s one of the leading causes of maternal death during pregnancy.
When chlamydia is symptomatic, what are we supposed to look for?
When symptoms are present, they usually include the following:
In women:
- – Painful urination
- – Abnormal vaginal discharge
- – Lower abdominal pain
In men:
- – Painful urination or discharge with urination
If chlamydia usually doesn’t cause symptoms in men or women, how does a person know he or she has it?
Today we have a number of excellent diagnostic tests that are quite accurate in detecting chlamydial infection, even when a person has no symptoms.
Increasingly, the preferred tests are those which are run on a sample of urine collected first thing in the morning. Chlamydia also can be grown in tissue culture or detected with less expensive tests, such as a smear that is stained and viewed under a microscope. In some cases, a blood test is used to detect evidence of past infection.
The availability of a urine test has created interest in widespread screening for this common but often asymptomatic infection. Urine tests can be used routinely to screen women who come in for an annual exam. Those who test positive can be treated and cured. Routine testing is recommended for all sexually active adolescents, as well as for women between the ages of 20 and 24 who have more than one sex partner.
How is chlamydia treated?
Treatment requires only a short course of antibiotics, taken orally. The treatment regimens recommended by the U.S. Centers for Disease Control and Prevention (CDC) include a single-dose option (azithromycin) or an antibiotic that’s taken twice daily for seven days (doxycycline). Either regimen will eliminate the infection within seven days in greater than 90% of patients.
What if I have a chlamydia infection I don’t know about? Should I – can I – be tested for this even if the exposure was years ago?
Chlamydia can hang around for years if it isn’t treated and can cause serious damage even when it’s asymptomatic. If you are seeing a doctor about a fertility issue, you should ask whether chlamydia screening has already been done. If it hasn’t, you can ask about getting a blood test that can tell you if you were infected in the past.
Can chlamydia be contracted through oral sex? If so, will the disease show up in the genital area?
Yes. Chlamydial infection of the mouth and throat can be contracted through oral sex, resulting in a sore throat and other symptoms. But this type of infection will not manifest itself in the genital area unless it is spread to the genitals through sexual contact. In addition, chlamydia in the mouth or throat is much less common than genital infection.
Posted in Protection & Common STD’s
November 3rd, 2016 by admin
Is gonorrhea still one of the “leading STDs?”
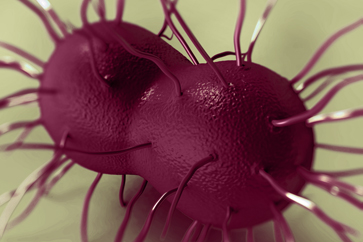
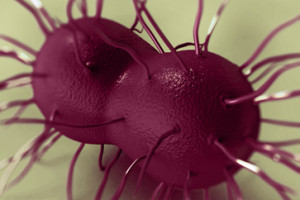 Gonorrhea is actually the number-one infectious disease among those classed as “reportable” by the CDC. In other words, any health care provider diagnosing a case of gonorrhea must report the case to the local public health authorities. This way, local health departments have accurate numbers to track the spread of gonorrhea in a given community and can take steps to contain it.
Gonorrhea is actually the number-one infectious disease among those classed as “reportable” by the CDC. In other words, any health care provider diagnosing a case of gonorrhea must report the case to the local public health authorities. This way, local health departments have accurate numbers to track the spread of gonorrhea in a given community and can take steps to contain it.
There are an estimated 800,000 new gonorrhea infections every year, about half of which are officially reported. Much like chlamydia, gonorrhea is a bacterial infection that is asymptomatic in up to three-quarters of women, yet it can damage the reproductive system over the long term, leading to infertility or other reproductive tract disorders. In men, the number of asymptomatic carriers is put at less than 5%.
How is gonorrhea transmitted?
Gonorrhea typically resides in mucous membranes such as the urethral canal and the vagina and is spread through unprotected intercourse–vaginal, oral or anal.
What are the symptoms of gonorrhea?
The word gonorrhea comes from the Greek term meaning “flow of seed,” referring to the discharge that is often found in those infected. When symptoms are present, they include the following:
In women:
- – Painful urination
- – Abnormal vaginal discharge
- – Bleeding between menstrual periods
- – Lower abdominal pain
In men:
- – Painful urination or discharge with urination
As an oral infection, gonorrhea can cause sore throat. Rectal symptoms may also occur in some cases, but these are relatively uncommon, especially in women.
How is gonorrhea diagnosed?
Typically, a health care professional swabs a woman’s cervix or a man’s urethra. The resulting sample can be tested by means of a culture or examined under a microscope with a stain that picks up evidence of gonorrhea. As with chlamydia, the future probably holds widespread use of urine tests for gonorrhea.
How is gonorrhea treated?
Gonorrhea can be cured with antibiotics–though in some cases treatment is complicated because some strains of gonorrhea are resistant to standard treatments. Several single-dose therapies are available as well as one-week regimens. Today’s treatments for gonorrhea cure the disease in more than 95% of patients with a single round of therapy. Others may require several different regimens before a complete cure is possible.
It seems like chlamydia and gonorrhea are very similar. Do health care providers have trouble telling them apart?
Based on symptoms alone, yes. What’s more, the two STDs are often found in the same people. Between 20 and 40% of those infected with gonorrhea also are infected with chlamydia. For this reason, it’s common practice in many clinics to treat both infections simultaneously. This often means single-dose therapy for gonorrhea, followed by a week of antibiotics for chlamydia.
Posted in Protection & Common STD’s

October 17th, 2016 by admin
What advice would you give to a person who is just becoming sexually active and wants to avoid getting an STD?
 In truth, there is no simple one-size-fits-all strategy for avoiding STDs. The best approach is probably to start by understanding the factors that determine your risk of acquiring an STD and then to think about the precautions you might take to lower it. As far as the first point, the basic principle is this: The more sexual partners you have, the more likely you are to acquire a sexually transmitted infection. Herpes is a good example. Among people who so far have had only one sexual partner 10% are infected. Among those with five to nine partners, 26% are infected, and among those with 10 to 49 partners, 31% are infected.
In truth, there is no simple one-size-fits-all strategy for avoiding STDs. The best approach is probably to start by understanding the factors that determine your risk of acquiring an STD and then to think about the precautions you might take to lower it. As far as the first point, the basic principle is this: The more sexual partners you have, the more likely you are to acquire a sexually transmitted infection. Herpes is a good example. Among people who so far have had only one sexual partner 10% are infected. Among those with five to nine partners, 26% are infected, and among those with 10 to 49 partners, 31% are infected.
Making decisions about your own risk for STDs requires that you know something about your partner’s history – how many people he or she has had sex with, any past history of STDs, and so on.
So what can you do – other than stay celibate?
The most effective all-around form of protection against STDs is the use of condoms for penetrative sexual acts such as inserting the penis in the vagina, anus, or mouth (fellatio). Condoms provide a barrier between the penis and the susceptible mucosal tissues of the vagina, cervix, anus, and mouth and stop the exchange of potentially infectious fluids such as semen, vaginal secretions and blood.
This is true of the traditional male latex condom and also the newer polyurethane condoms, including the female condom that came onto the market in the mid-1990s. Natural membrane condoms do offer some protection against STDs, but during the 1980s, research showed that microscopic pores in these devices were actually larger than some of the sexually transmitted viruses, such as hepatitis B and HIV. For this reason, public health officials began to specify latex condoms in their efforts to stop the spread of HIV and other STDs. The newer polyurethane condoms haven’t been studied as thoroughly as latex condoms, and they appear to have higher failure rates. The U.S. Centers for Disease Control and Prevention recommend latex condoms for STD prevention over condoms made with other materials.
When are condoms effective and when aren’t they?
Used properly and consistently, condoms can stop the spread of many infections, including chlamydia, gonorrhea, trichomoniasis, syphilis, hepatitis, and HIV. Their effectiveness against the viral STDs herpes and HPV, however, is not completely known. One reason is that these two STDs can be spread readily from lesions that occur in places not covered or protected by a condom. For example, even if he were wearing a condom, a man with a herpes sore on the scrotum would put a female partner at risk, because the close contact of intercourse might allow virus to spread from scrotum to labia.
The phrase “properly and consistently” also bears on the effectiveness of condoms. Condoms made of any material can fail in a number of ways if misused. They can slip off if lubricated on the inside, for example, or if an erection subsides. And latex condoms can be damaged by use of oil-based lubricants such as hand creams, skin lotions, and petroleum jelly (Vaseline). The female condom may take practice to insert correctly and can be inserted incorrectly or dislodged in a number of ways.
This is not to say you have to be a rocket scientist to use condoms correctly. You do not. They are inexpensive, widely available, and easy to use. It’s simply a good idea to familiarize yourself with the package insert of your brand to make sure your condom habits are correct.
What are the most important guidelines on using condoms correctly?
- – Store condoms in a cool, dark place. Heat and humidity are especially bad for latex.
- – When opening a condom wrapper, be careful not to damage the condom itself with your teeth or fingernails.
- – When putting on a condom, hold the tip–the part where semen will be deposited–between the thumb and forefinger and squeeze out the air, including the air in a reservoir-style tip.
- – Unroll the condom over the entire shaft of the penis.
- – After penetrative intercourse, remove the penis while it’s still erect; otherwise the condom may slip off prematurely.
- – Use a new condom for each act of intercourse.
What about spermicides?
Spermicides, as the term implies, were developed as a contraceptive–to kill sperm. It was later discovered in laboratory experiments that they also kill some of the microbes associated with STDs, and research has shown that they can prevent the transmission of chlamydia and gonorrhea. Against this backdrop, some have advocated the use of spermicides as a form of STD prevention for those who will not or cannot use condoms. This is still a controversial recommendation, however, because if used often, spermicides can cause irritation in the vagina that may actually increase the risk of getting certain infections. In addition, there are questions about the proper dose needed to neutralize or kill STDs, which may be different from the dose that works to kill sperm.
Is oral sex safer – that is, less likely to spread STDs – than other kinds of penetrative sex?
In a general sense, yes. Most STDs have the potential to be spread through oral sex, most commonly resulting in sore throat and other oral symptoms. But it’s also true, as a rule, that sexually transmitted infections in the mouth and throat are much less likely to develop than genital infections, which suggests a lower risk from oral sex. This may be because the oral cavity is a less hospitable environment for sexually transmitted microbes than the genital tract, though this remains a matter of speculation.
Oral sex, however, does account for substantial numbers of genital herpes infections and is still considered a risk for HIV, specifically because of the potential for cuts or abrasions on the gums that might give HIV an open door into the bloodstream. Hepatitis viruses, in some cases, also can be spread through oral sex.
In sum, the risk from oral sex is lower than having penetrative vaginal or anal intercourse, but it isn’t zero. For this reason, people practicing oral sex with a partner who might carry an STD are advised to use condoms for fellatio or barriers such as dental dams or plastic wrap for cunnilingus.
What’s a dental dam?
Originally developed for use in oral surgery, dental dams are square pieces of thin latex that can also be used to prevent the exchange of bodily fluids during oral sex. A dam must be held in position over the vulva or anus during oral stimulation, always keeping the same side of the dam against the body.
Dental dams can purchased through various sex boutiques and catalogs. Some authorities recommend plastic wrap as an alternative to dental dams because it’s easier to get and can be used in larger sizes.
What is outercourse? How safe is it?
Outercourse is a term coined in the 1980s as part of the effort to prevent the spread of HIV by encouraging safer sex. It refers generally to practices that can give sexual pleasure without creating the risks implicit in vaginal, oral, or anal sex. Examples include sensual massage, fantasy, self-masturbation, pleasuring a partner with the hands, and other forms of sex play.
Safety is a relative issue. Although much safer than penetrative sex, some forms of outercourse do carry the risk of skin-to-skin transmission of herpes or genital HPV.
What if a person already has an STD? How can the person’s partner get protection?
Again, there’s no universal measure to stop all STDs. With infections that can be cured with medication, the person being treated should refrain from having sex until the infection is cleared.
With chronic infections such as genital herpes or genital HPV, it’s wise to avoid contact with lesions, but as we stressed earlier, these infections can be transmitted even when no obvious lesions are present. That’s why for herpes and HPV you should discuss the issues with your partner and decide which precautions, if any, you need to take.
What about a woman who has had only a couple of sexual partners and whose annual gynecological exams have always been normal. Should she still be concerned about having a sexually transmitted disease?
The good news is that statistically a women with only a couple of partners does indeed stand a lower chance of contracting an STD than someone who has a larger number of partners. The fact that her annual Pap smears and gynecological exams have been normal and that she reports no troubling symptoms raises the likelihood that she is free of STDs.
On the other hand, as we have stressed, a number of very widespread STDs tend to be asymptomatic. And annual gynecological exams do not routinely include screening for STDs. Therefore, one can’t be entirely sure about being free of STDs based simply on routine care. Chlamydia, as an example, is both extremely common and frequently silent. And as we said earlier, it can also affect a woman’s ability to have children, which is why it’s a good idea for all sexually active women to be screened for chlamydia. Screening can also be done for other STDs in their asymptomatic phases, including herpes. It’s a good idea to talk with your health care provider about your situation and which, if any, tests might be needed.
How can I tell if my prospective sexual partner has an STD?
You can’t always tell, but you can always ask. If you’re contemplating a sexual relationship with a new partner, you should ideally discuss past sexual experiences and sexually transmitted diseases–first. For most people, the concern driving this discussion and driving the need for condom use or other “safer sex” approaches has been the fear of AIDS. But as long as you’re talking about AIDS, you might as well talk about the other STDs that are more common than AIDS. Of course, talking about it is no guarantee. There are those who will lie, and those who quite honestly don’t know that they carry an STD. Most people who have genital herpes, for example, never experience obvious symptoms. The same is true of chlamydia.
If you are sexually involved with someone, don’t turn a blind eye to any type of rash, sore, or ulceration in the genital area. Likewise, someone who has a cold sore or fever blister on or around his or her lips poses a risk of transmitting herpes through oral sex. If you are frequently having sex with people you don’t really know and with whom you have not had an in-depth “safer sex” discussion, the proper use of condoms or other barriers (such as dental dams) is in order.
How do I tell my partner I have an STD?
Telling a prospective partner you have an STD can be difficult for those who have a persistent viral infection such as herpes, genital HPV or hepatitis. Bringing up your personal history of infection is probably easiest in the context of a more inclusive safer-sex conversation. Before you become involved with anyone sexually, you deserve to know something of his or her sexual history. You have news to share, and perhaps he or she does too.
Choose a quiet, private place with a relaxed atmosphere and try to ensure that you have ample time for discussion. It’s normal to feel apprehensive about telling, and it will be normal for your partner to feel apprehensive about the possibility of contracting an infection. Remember that most people have a poor understanding of what STDs are, how common they are, how they’re transmitted, and how they’re treated.
Be prepared to answer questions, and don’t expect your partner to come to terms with the issue on the spot. Give him or her time to take it all in.
Posted in Protection & Common STD’s

August 27th, 2016 by admin
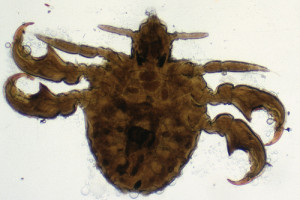
Are scabies and public lice the same thing?
No, though they have several things in common. Both are parasites that infect the skin and are spread through close physical contact, though not exclusively sexual contact. An example would be the sharing of bed clothes or towels. Both parasites cause itching, and both are treated with topical drugs that essentially poison them.
Scabies is an infection caused by the itch mite, a sort of microscopic tick that burrows into the skin and lays eggs, which then hatch and develop into adults within 10 days. Symptoms include itchy burrows on the hands and wrists in a majority of cases. These burrows also can be found on the chest, buttocks, thighs and penis. Scabies is seldom found on the neck or face.
Lice, on the other hand, come in three species that infect humans–head, body and pubic lice. All three are visible to the naked eye and lay eggs (nits) that are visible, usually at the base of hair follicles. As you might guess, pubic lice (also called crabs) are the species most likely to be sexually transmitted.
How is scabies diagnosed and treated?
For diagnosis, a health care provider will take a sample of the burrows and examine it under a microscope for the characteristic wavy shape of the burrow. Treatment consists of applying a topical ointment or cream over the entire body from the neck down. The treatment is washed off after 8 to 12 hours. Antihistamines may be used to quell the itching that sometimes continues after treatment. Frequently, the infected person’s family members, who are at high risk for exposure, are also treated, even if they have no symptoms.
How are lice diagnosed and treated?
Pubic lice usually are identified based on a medical history and physical examination for either the lice or nits. They can be treated with a variety of topical drugs and shampoo preparations that are applied to the skin and then washed off after a specified number of hours. It’s important to remove the medication, because it can cause a rash or skin problems. Some of the medications used for scabies are also used for lice, including permethrin (Elimite®, Nix ®) and lindane (Kildane®, Scabene®). Be careful to follow your health care provider’s instructions about which type of formulation to use and how to apply it.
What about infestation in the household? How do you get rid of the lice and scabies that may not be killed by medication?
The house does not have to be fumigated, but bedding and clothing should be decontaminated. Wash them in hot water or send them to be dry cleaned. Lice and crabs will generally die if deprived of a human host for three days.
Posted in Protection & Common STD’s



 Chlamydia is a unique type of bacterium that attaches itself to healthy cells and draws on these cells for the elements necessary to grow and invade other cells. It does not belong to the group of bacteria that are normally found in the genital tract but is transmitted sexually through contact with secretions such as semen and vaginal fluids.
Chlamydia is a unique type of bacterium that attaches itself to healthy cells and draws on these cells for the elements necessary to grow and invade other cells. It does not belong to the group of bacteria that are normally found in the genital tract but is transmitted sexually through contact with secretions such as semen and vaginal fluids.
 Gonorrhea is actually the number-one infectious disease among those classed as “reportable” by the CDC. In other words, any health care provider diagnosing a case of gonorrhea must report the case to the local public health authorities. This way, local health departments have accurate numbers to track the spread of gonorrhea in a given community and can take steps to contain it.
Gonorrhea is actually the number-one infectious disease among those classed as “reportable” by the CDC. In other words, any health care provider diagnosing a case of gonorrhea must report the case to the local public health authorities. This way, local health departments have accurate numbers to track the spread of gonorrhea in a given community and can take steps to contain it.
 In truth, there is no simple one-size-fits-all strategy for avoiding STDs. The best approach is probably to start by understanding the factors that determine your risk of acquiring an STD and then to think about the precautions you might take to lower it. As far as the first point, the basic principle is this: The more sexual partners you have, the more likely you are to acquire a sexually transmitted infection. Herpes is a good example. Among people who so far have had only one sexual partner 10% are infected. Among those with five to nine partners, 26% are infected, and among those with 10 to 49 partners, 31% are infected.
In truth, there is no simple one-size-fits-all strategy for avoiding STDs. The best approach is probably to start by understanding the factors that determine your risk of acquiring an STD and then to think about the precautions you might take to lower it. As far as the first point, the basic principle is this: The more sexual partners you have, the more likely you are to acquire a sexually transmitted infection. Herpes is a good example. Among people who so far have had only one sexual partner 10% are infected. Among those with five to nine partners, 26% are infected, and among those with 10 to 49 partners, 31% are infected.

